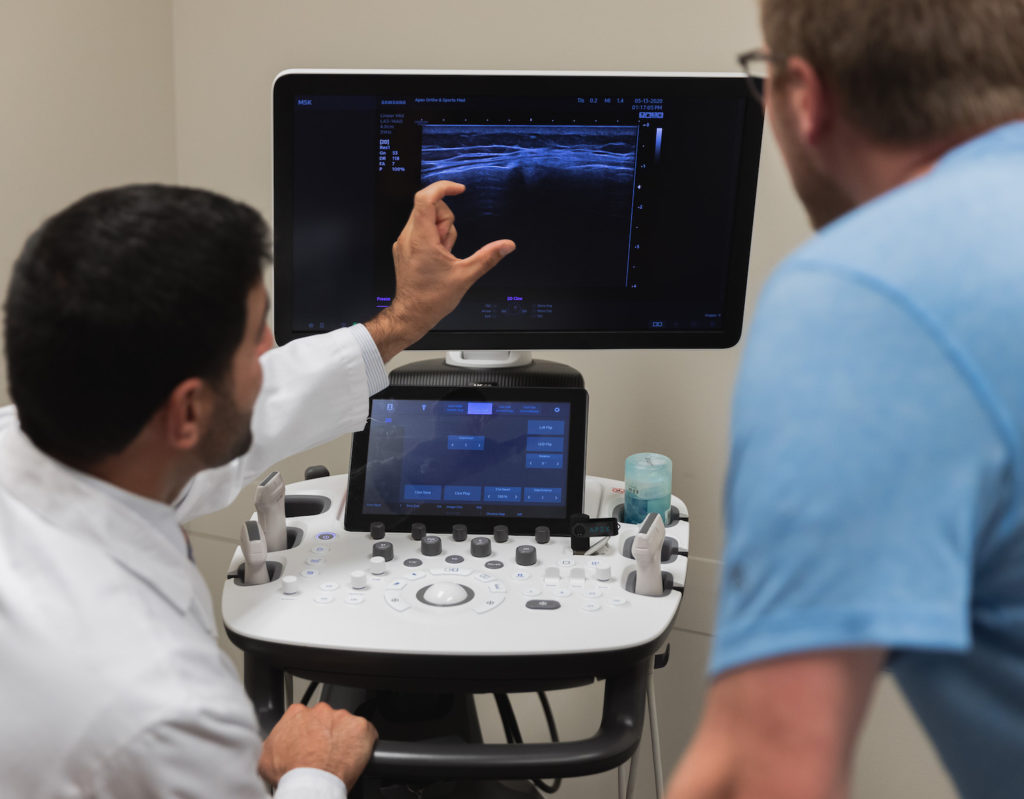
 KCOA offers total joint revisions in Kansas City for patients who have found that other options no longer work for them.
KCOA offers total joint revisions in Kansas City for patients who have found that other options no longer work for them.
Total joint arthroplasties are surgeries done to alleviate the symptoms and pain of osteoarthritis. Most commonly done in the knee, hip, and shoulder, these surgical procedures replace arthritic joints with prosthetic implants that function as a new joint.
Total joint arthoplasties in Kansas City by KCOA have excellent success rates, and with new and improved surgical techniques and medical advancements, even total knee replacements can last 15 to 20 years in the majority of patients!
That being said, there are times when a second or even third surgery is required if the original replacement fails.
Signs of a failed total joint arthoplasty could include increased pain, decrease in function, redness, swelling, or incisional drainage. But how (and why) does a total joint arthoplasty fail?
A joint arthroplasty can fail for a few reasons.

First, arthoplasty can fail from normal wear and tear.
Although most implants are determinedly implanted at the time of surgery, they may become loose over time. This can be exacerbated by vigorous exercise that involves pounding on the joint (such as excessive running), traumas, age, or weight (obese patients have a higher risk of loosening).
Overall, the more friction that occurs as the joint components rub against each other, the more the surface of the prosthetic can begin to wear.
During this process, minuscule particles accumulate and as the body naturally attempts to digest them, aseptic (or uninfected) loosening occurs. To diagnose this, a test called a bone scan is ordered and will show areas where loosening may be occurring.
Secondly, arthroplasties can fail due to infection.
Anytime foreign materials are introduced into the body, there is a risk of bacterial spread. Nationally, the risk of infection after a total joint procedure is less than 1%. But while it is rare, it is also a life-changing complication.
Many precautions are taken to prevent this: a completely sterile field during surgery, antibiotics at the time of and after surgery and tight wound closure with clean surgical dressings.
If just a superficial infection is suspected, a much smaller washout procedure with exchange of the plastic parts of the replacement can be done.
If the infection is suspected to be deep, or the original washout surgery is unsuccessful, patients must have surgery remove the original prosthetic and have an antibiotic cement spacer placed for 6 weeks while receiving IV antibiotics.

After that 6 week period, if all inflammatory markers are down, then a new total joint is put into place. Infection is diagnosed by firstly getting a panel of labs to evaluate for inflammation in the body, namely a CBC, CRP and SED rate. If these labs indicate infection, then an aspiration is taken from the joint and tested directly.
Revisions can also be required for instability, or if the artificial joint dislocates. This is a painful occurrence and can cause unsteadiness. This can be due to improper alignment or from ligament laxity.
Lastly, a fracture can occur.
A revision can be necessary if a fracture occurs that is around the implant and disrupts the fixation or stability of the implant. It is difficult to prevent these peri-prosthetic fractures as they are often due to falls or other traumas.
If you’re looking for total joint revisions in Kansas City, KCOA Orthopedics can help.
KCOA has a professional, seasoned team of orthopedic surgeons on staff to walk you through more information about total joint revisions in Kansas City. We have also learned a variety of strategies to help prevent complications or failures of total joint arthoplasties.
Contact us today to book your appointment or with any other questions you may have about total joint revisions.