Achilles Tendon Repair in Kansas City
Achilles Tendon Repair
Getting you back on your feet
Understanding the Basics Behind Achilles Tendon Repair
What is Achilles Tendon Repair?
Whether you’re an athlete on the field or just going about your daily life, Achilles tendon injuries can happen to anyone.
These injuries can appear in the form of tendonitis or a complete rupture of the tendon itself. The causes of Achilles injuries range from overuse and repetitive motions to sudden, forceful strain.
If you’re suffering from tendonitis, or believe you’ve suffered a complete tear of the Achilles tendon, it’s vital to seek guidance from experienced orthopedic specialists. At Kansas City Orthopedic Alliance, we can ensure that you receive a proper diagnosis and a comprehensive treatment plan suited to your needs and challenges. With over 140 years of combined service, we utilize the best technologies and techniques customized to each patient.
After your initial examination with a KCOA physician, we will recommend the best treatment for your needs. Our practitioners provide the comprehensive care you need so you can return to the activities you enjoy.
Choosing Achilles tendon repair in Kansas City is a decision that typically involves guidance from your primary care doctor and orthopedic physician.
When you choose Kansas City Orthopedic Alliance, one of our highly-trained orthopedic foot and ankle specialists will conduct an initial evaluation to better understand your condition. After a complete review of your results, your provider will discuss whether Achilles tendon repair is the best treatment option for you.
Other common symptoms of Achilles injuries include:
- Pain that stretches down your leg into your heel
- Pain that worsens through activity
- Soreness
- Stiffness
- Swelling
- Thickening of the tendon
- A sudden popping sound with sharp pain
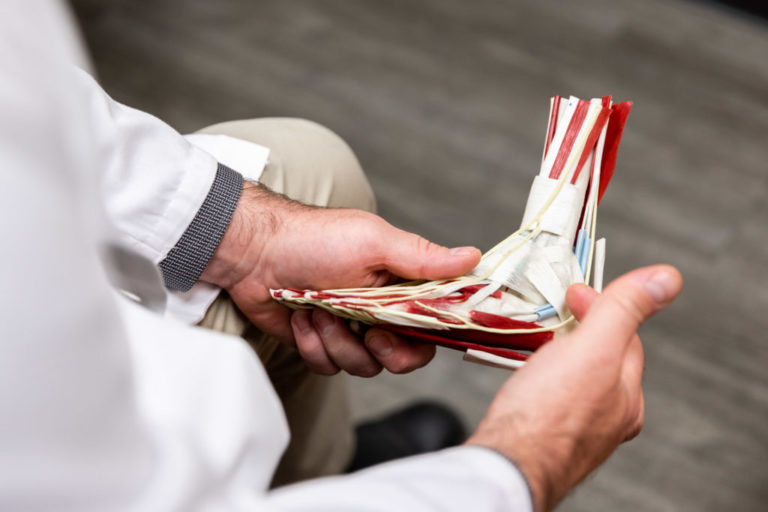
Kansas City Orthopedic Alliance Achilles tendon Assessment
Assessing the Injury
Determining the proper Achilles tendon repair treatment starts with an assessment from one of our experienced providers.
You can think of foot and ankle pain as a spectrum, with some instances being more severe than others. The KCOA orthopedic specialists always focus on each patient and their concerns before creating a treatment plan.
Therefore, during your initial appointment, we will often ask questions such as:
- How did your injury occur/what was the mechanism of injury?
- Did you notice or hear a popping sound at the time of your injury?
- Is walking or running painful or limited by the injury.
- Has your pain progressed or worsened recently?
- Have you experienced any tingling or numbness in your foot that makes tasks difficult?
- Have you noticed any change in your symptoms that has made it more challenging to function?
- What are your lifestyle goals?
- How has pain affected those goals?
The answers to these questions help shape the next steps of the assessment process and guide our physical examination. After a proper assessment, we often begin with a physical examination to help determine the origin point of your pain. In some cases, advanced testing may be required for a full diagnosis.
Examination
X-Ray
Also called radiographs, an X-ray captures a picture of the ankle, heel, or lower leg. Orthopedic physicians may order an X-ray to rule out the possibility of a fracture (broken bone), osteoarthritis, or other bone-related conditions.
Magnetic Resonance Imaging (MRI)
MRI captures images of muscles, bones, intervertebral discs, and tendons to help provide information other tests can’t detail. During an MRI, you will lie on a table that slides into a tube-shaped scanner. The machine creates a magnetic field around you, using pulsed radio waves to form the MRI images.
Symptoms
Common Signs and Symptoms of Foot & Ankle Injuries
With so many different parts working together in your feet and ankles, there are many potential causes of pain. And each of those causes has a unique set of symptoms.
Achilles injuries often cause pain and swelling in your heel, making it difficult to walk or bend downward. In less severe cases, you may feel pain and stiffness in the heel. When a patient visits one of our KCOA offices, a skilled orthopedic specialist will ask you questions regarding your symptoms, what aggravates/alleviates your symptoms, and whether you have attempted prior therapies. Next comes a thorough physical exam. We will then review any images you bring with you and/or take new images. After determining the cause of your pain or loss of function, we will discuss the best treatment options to meet your needs.
Causes
Causes of Foot & Ankle Pain
The body has different kinds of joints, and they all face different challenges. The foot and ankle combine for a complex region of the body, totaling 26 bones and 33 small joints that experience daily wear and tear. Soft tissue protects the joints and bones, and is made up of muscles, tendons, ligaments, nerves, and blood vessels.
The Achilles tendon is part of this soft tissue system and is the largest tendon in your body. It connects your calf muscles to your heel bone. It allows you to push off forcefully with your toes, like when you jump, run or raise your heels up off the ground.
The most common cause of tendonitis is repeated motion, a spike in activity or simply the daily wear and tear that accumulates from years of activity. When your Achilles tendon tears, however, it’s often because of a sudden strong force. Many athletes rupture their Achilles tendons due to non-contact injuries, such as sudden movements or pivots.
Treatment Alternatives
Generally, surgery is not the first choice for treatment at Kansas City Orthopedic Alliance. If we can treat your Achilles tendon issue with more conservative treatments, we will do so. We typically exhaust all non-surgical options before recommending surgery.
Non-surgical treatments for Achilles tendon injuries include:
Physical Therapy
Movement can actually reduce pain and encourage healing in the Achilles tendon, as movement increases circulation and supplies other nutrients that support joint health and function. Stretching and flexibility exercises, strengthening exercises, deep tissue massages, and cryotherapy may be helpful.
Medications
Your doctor may recommend over-the-counter NSAIDs (Non-steroidal anti-inflammatory drugs, such as Advil) or prescription medications. Especially with NSAIDs, you should always talk to your doctor to ensure they are the right treatment for you.
Immobilization
Immobilization involves the use of casts, braces and walking boots to allow the affected area to heal. With immobilization, we can protect the Achilles tendon and allow the area to heal while reducing pain and swelling.
Regenerative Medicines
Regenerative medicines like stem cell injections or platelet-rich plasma can help nourish worn or damaged tissue. This option works best if you have mild-to-moderate Achilles pain or minor tearing of the tendon.
F.A.Q.
Frequently Asked Questions
Kansas City Orthopedic Alliance is here to help.
Our care is personal. Our team is knowledgeable. And we’re more available than ever.
With access to board-certified specialists across Kansas City, we have the tools to meet almost every musculoskeletal condition.
Our Locations
Overland Park, Kansas
10777 Nall Ave Suite 300 Overland Park, KS 66211Leawood, Kansas
3651 College Blvd. Leawood, KS 66211Kansas City, Missouri
Saint Luke's Medical Plaza #1 4320 Wornall Rd., Ste. 610 Kansas City, MO 64111Belton, Missouri
Belton Regional Campus 17067 S Outer Rd #301 Belton, MO 64012Blue Springs, Missouri
St. Mary’s Medical Center, Main Entrance 203 NW R.D. Mize Road, Suite 200 Blue Springs, MO 64014Shawnee Mission, Kansas
7450 Kessler St ste. 140 Merriam, KS 66204Prairie Star (Lenexa, Kansas)
Prairie Star 23401 Prairie Star PkwyBldg. B, Ste. 220 Lenexa, KS 66227