The right orthopedic facility ensures you not only return to play faster, but also maintain optimal joint and muscle health to continue on. Whenever an injury strikes, it’s key to take the necessary precautions and steps for faster recovery. However, the orthopedic sports physicians you choose hold a crucial piece of your success.
KCOA is a top sports clinic in Kansas City focused on providing the best care to athletes of all ages. Regardless of your injury or condition, we find treatment solutions that will work best for you.
What does a top sports medicine clinic in Kansas City do and treat?
A top sports medicine clinic implements orthopedic medical practices to diagnose and treat sports-related musculoskeletal conditions. While many injuries aren’t limited to athletes, repetitive physical activities from sports make the onset of certain conditions more prevalent.
Many athletes work with athletic trainers or other health care providers, and a sports medicine physician helps fill in those gaps when they need advanced diagnosis and treatment. For example, you may require imaging to specify the difference between a stress fracture and joint and muscle overuse. A physician can utilize tools such as X-rays and MRI scans to gain insight into your injury.
Whenever you injure yourself, it’s important to seek help immediately, especially if pain continues or worsens. Without medical attention, you could unknowingly cause irreparable damage that could pull you away from your sport.
Common sports-related conditions include:
- Ligament sprains or tears
- Tendonopathy
- Tendon tears
- Muscle strains
- Knee injuries
- Rotator cuff injuries
- Spinal injuries
- Concussion-related brain injuries
- And more
Since not all injuries are the same, nor do they require the same treatment, you should always search for a sports medicine clinic that centers on you. While we can’t explain all of your possible conditions(your orthopedic physician can give you more specific information during your initial appointment), we will briefly describe common injuries based on location.
Concussions
Concussions are mild traumatic brain injuries caused by direct blows to the head or acceleration forces. Despite what some people may believe, concussions do not result in structural damage. Instead, they are neurochemical injuries that temporarily disrupt brain function. Due to their unique nature, concussions require strict management and return to play guidelines to optimize athlete safety, promote brain health, and ensure a full recovery.
Whenever you believe you have a concussion, there won’t be a single test that would diagnose the condition. Rather, your physician diagnoses your injury based on specific signs. If you develop symptoms such as temporary loss of consciousness, headaches, or dizziness directly after a head injury, then it may be a concussion. However, symptoms generally improve and resolve themselves within a few days to weeks.
Just because your symptoms may disappear, however, it doesn’t mean you shouldn’t take the proper precautions. The best management requires a gradual return to activities, even those outside of your sport such as work and school (though this depends on the severity of your injury). Sometimes, medications or supplements can improve your symptoms as your brain heals. Ultimately, your orthopedic physician will determine whether that would be the right path for you.
One of the biggest concerns during healing is the risk of a second concussion. If you sustain another concussive blow while your brain is still recovering, you could experience significant complications—some even long-term or potentially life threatening. Therefore, you should never rush your recovery. That means you will have to remain benched from your sport until you are asymptomatic, can tolerate all cognitive school and/or work activities, and have succeeded with your gradual return-to-play plan.
Both Dr. Khadavi and Dr. Moore at KCOA provide accurate diagnoses and effective treatments for sports related concussion.
Shoulder Injuries

Shoulder injuries can be quite common, especially for pitchers and other types of throwers. Any condition that affects joints, muscles, ligaments, tendons, nerves, and other physical structures in the shoulder may require medical attention. These injuries and conditions include:
- Rotator cuff tears
- Labrum tears
- Joint instability
- Shoulder dislocation
- And other sports-related injuries
An orthopedic shoulder specialist can assist with finding non-operative management treatment options. If your physician is also a surgeon, they can implement operative treatment solutions to repair the injury and manage pain. For athletes, the main goal is to produce outcomes that maximize their functionality for a safe return to play.
When you visit a top sports clinic, you will undergo a detailed evaluation of your shoulder injury followed by a physical examination. Your physician may need further testing such as X-rays, ultrasound, or MRI to accurately diagnose your injury.
Shoulder specialists, such as Dr. Van den Berge at KCOA and Dr. Michael McCabe typically lean toward conservative, non-operative measures as their primary treatment approach. Surgical management options may be part of the end discussion, but a majority of sports-related shoulder injuries do not require surgery, especially not as the first treatment option.
What You Should Know Before Visiting an Orthopedic Shoulder Specialist.
A few examples of conservative shoulder injury treatments include:
- Physical therapy tailored to your diagnosis
- Modifications in your activities
- Braces and slings
- Pain medication
- Steroid injections
- Orthobiologic injections (such as platelet-rich plasma or bone marrow aspirate concentrate)
Ultimately, physicians will align their management recommendations with your goals. Therefore, two people with the same diagnosis may undergo two different management plans. For example, a competitive athlete may need more intensive management to resume play, whereas a more recreational athlete may simply require more functionality and less pain through less intensive treatments.
Nerve & Spinal Injuries
“Nerve injury” is a broad term that encompasses a variety of conditions. So before your physician develops a treatment plan, he or she must understand which type of sports-related nerve injury you have. At KCOA, our newest physician, Dr. Moore, specializes in diagnosing and treating peripheral nerve injuries.
Learn more about peripheral nerve injury evaluation and management.
Nerve entrapments
Nerve entrapments are a type of mononeuropathy. That means the injury occurs to a single peripheral nerve at a specific location in your body. Entrapment neuropathies (also called compression neuropathies) include diagnoses such as carpal tunnel syndrome and cubital tunnel syndrome. In an ideal anatomical course, nerves travel in smooth channels or cushioned spaces between muscles, ligaments, and bones. When those spaces around a nerve narrow, it can cause nerve compression and irritation, which leads to pain and discomfort.
The specific symptoms of nerve compression depend on the nerve involved and what it innervates. However, common symptoms of nerve compression include:
- Pain
- “Pin-and-needles” sensation
- Numbness
- Muscle weakness
Radiculopathy
While the term “radiculopathy” may be new for you, people often refer to the condition as a “pinched nerve,”. However, the terminology sounds more aggressive than what is actually occurring anatomically.
Radiculopathy relates to the irritation of a spinal nerve (the large bundle of nerves that exits the spine). Cervical radiculopathy affects the cervical spinal nerve at neck level, while lumbosacral radiculopathy (also known as “sciatica”) affects the lumbosacral nerve at the low back level.
Disc bulges/herniations or spinal degenerative changes that cause narrowing and inflammation at the spinal nerve exit point typically result in radiculopathies. In less common scenarios, the condition may stem from spine tumors or infections.
Complexities in the history and examination for someone with radiculopathy affects management. Therefore, if you experience symptoms such as numbness, tingling, or focal weakness in the affected limb, you should always visit a top sports clinic with highly experienced orthopedic doctors.
Classically, radiculopathy generates radiating extremity pain that spreads down the arm or leg rather than stagnant neck or back pain. This happens due to how the body interprets nerve irritation. Keep in mind that pain may worsen with certain activities, so it is best to take a break from your sport until your physician clears you.
Hand and Wrist Fractures

Hand and wrist fractures involve one or multiple broken bones and can range in severity. As with other areas of the body, fracture-causing injuries may come from anything—falling, sports, car accidents, jammed fingers, or even yard work. Treatment typically involves casting for a designated time period.
Here’s why:
A broken bone creates a gap at the fracture site. Bone healing cells have to jump across the gap to knit the bone together, but if the bone constantly moves, those cells can’t cross and heal the fracture. A cast (or even a splint in some cases) holds the bones together so healing can continue properly. Without a cast or splint, bone healing cells will build bone everywhere due to too much motion. As a result, healing could take a lot longer.
While most fractures heal through conservative treatment options, some patients may require surgery based on two main factors:
- Abnormal bone alignment that cannot heal
- Deformities that would affect a patient’s ability to use the hand/wrist optimally
During a visit, your physician can better understand the extent of your fracture and recommend treatment options. At KCOA, Dr. Deardorff caters her practice to many conditions and sports-related injuries involving the hand and wrist.
What You Should Know About Hand & Wrist Fractures
If you think you have a broken bone, it’s vital that you visit a physician as soon as possible. Waiting for treatment (or avoiding treatment altogether) could lead to misaligned healing, and your doctor may have to re-break the bone to fix the issue.
How do I know whether I have a fracture?
Unless the break is severe, you may not know for sure that you have a fracture without a medical exam and diagnostic studies. However, you can watch for symptoms such as:
- Pain
- Bruising
- Swelling
- Inability to move joints
- Tenderness
- Obvious deformities
Not all hand and wrist fractures are the same nor do they show the same symptoms. While there are several types of hand and wrist fractures, a majority of fractures fall into two main categories:
- Distal Radius/Ulnar fractures
- Scaphoid fractures
Distal Radius/Ulnar fractures
Your forearm (below the elbow) comprises two bones—the radius and the ulna—which connect to the wrist bones. The word “distal” signifies the end furthest from the center of the body. Therefore, a distal radius or ulnar fracture is a break at the end of the bone near the wrist. This type of fracture often occurs from a fall, making it the most common type of wrist fracture.
Symptoms include:
- Pain
- Wrist swelling
- Wrist deformity
- Inability to flex or rotate the wrist
Scaphoid fractures
The scaphoid is a small, oddly shaped bone that makes up part of the wrist (there are eight total bones). It sits at the bottom of the thumb closest to the radius bone of your forearm.
It’s common to miss scaphoid fractures, so it’s very important to seek medical help if you have a wrist injury. Left untreated, the fracture may not heal appropriately and can lead to arthritis.
Similar to distal radius fractures, scaphoid fractures often happen from a fall, but the symptoms are milder. Since scaphoid fractures typically only result in minimal swelling and some pain, many people mistake them for wrist sprains.
Hip Injuries
Hip pain can be a major hindrance and concern for athletes, regardless of the sport. Specifically, hip impingement is one of the leading hip conditions among athletes and occurs when the femoral head (top of the leg bone) abnormally rubs against the acetabular socket (the indention where the leg bone meets the hip bone).
Typically, people have a nice slope along the head and neck of the leg bone, which allows the bone to fit properly into the socket. However, this does not always happen. Sometimes, extra bony growths may form that affect how the leg bone connects and moves within the hip socket. These bony growths often appear as bumps and can emerge in two main locations.
- Cam Impingement: Cam impingements are bony growths that appear around the head or neck of your leg bone. It is also the most common type of impingement.
- Pincer Impingement: Pincer impingements are growths that appear on the hip socket, or can happen when the socket sits at an abnormal angle.
Hip impingement pain can happen any time between the teenage years to middle age and beyond, since adolescent development may induce bumpy growths. Younger children rarely face hip impingement.
ACL Tears

ACL tears happen to many athletes, especially those who engage in high-intensity sports such as football, basketball, and soccer. An ACL tear comes from a sprain in one of the major ligaments in your knee. If you ever experience a tear, you may notice a popping sound when the injury occurs, followed by swelling, pain, or feeling like your knee is “giving out.” At KCOA, Dr. McCabe and Dr. Van den Berghe and Dr. David Clymer often treats ACL tears and other knee injuries in younger athletes.
ACL may originate from:
- Sudden change in movement
- Pivoting on a planted foot
- Landing awkwardly from a jump
- Direct hits to the knee (common in football)
- Abrupt stops
As with any sports-related injury, ACL tears range in severity. So while some people may recover with bracing and physical therapy, others may require a surgical repair. The only way to understand the severity of a knee injury is by visiting a top sports clinic for an examination.
Learn about knee scope surgery for ACL tears.
Foot & Ankle Injuries
Many sports-related injuries lead to foot and/or ankle pain. With strong ligaments to support the joints, the foot and ankle can move properly without causing pain. But whenever anatomical elements become injured or have abnormalities, that can greatly impact someone’s daily life, including the ability to participate in sports.
Your Guide to Orthopedic Foot & Ankle Care
There are a variety of foot and ankle sports injuries, but ankle fractures, tendon tears, and chronic ankle sprains are common. For those in the Kansas City area, Dr. Kneidel at KCOA specializes in the diagnosis and treatment of all three injuries (and other foot and ankle issues).
Ankle fractures
An ankle fracture occurs when one or more of the ankle bones break. Fractures range in severity from minor breaks to severe breaks that require you to remain non-weight bearing for an extended period. Broken ankle bones may also cause ligament damage, which further destabilizes the joint.
Ankle fractures can happen to anyone, no matter the age or activity level. The injury could come from sports, falls, car accidents, sudden twists or rotations, and more. Especially with older people, activity level can impact the probability of ankle fractures.
Ligament tears
Tendon tears may come from trauma or repetitive motions that add pressure to the ankle. The severity of the tear plays a huge role in the treatment options. Some may benefit from bracing and injections, while others may have to undergo surgery.
Chronic ankle sprains
Ankle sprains are a tear of one or two ligaments, and the severity lies on a broad spectrum. For instance, you could have a partial tear or a complete tear. About 95% of the time, people recover from ankle sprains and return to their normal activities. However, there are times when a person may have neglected proper treatment or failed to rehab the joint. When that happens, the joint isn’t protected enough to allow the ligaments to repair themselves, thus leading to instability and chronic sprains.
Find the Right Orthopedic Physician for Ankle Sprains
Treatment Options at Top Sports Medicine Clinics for Sports-Related Injuries

Most sports-related injuries do not require surgical intervention and typically heal within a few weeks to months. To ensure your injuries heal, it’s vital to follow your treatment plan and take the recovery process seriously. Even if you’re anxious to return to play, getting back to the field too soon could cause more harm down the road.
At KCOA, our physicians work with you to find treatment solutions that help manage your pain, increase stability, and prevent further injuries. These options include:
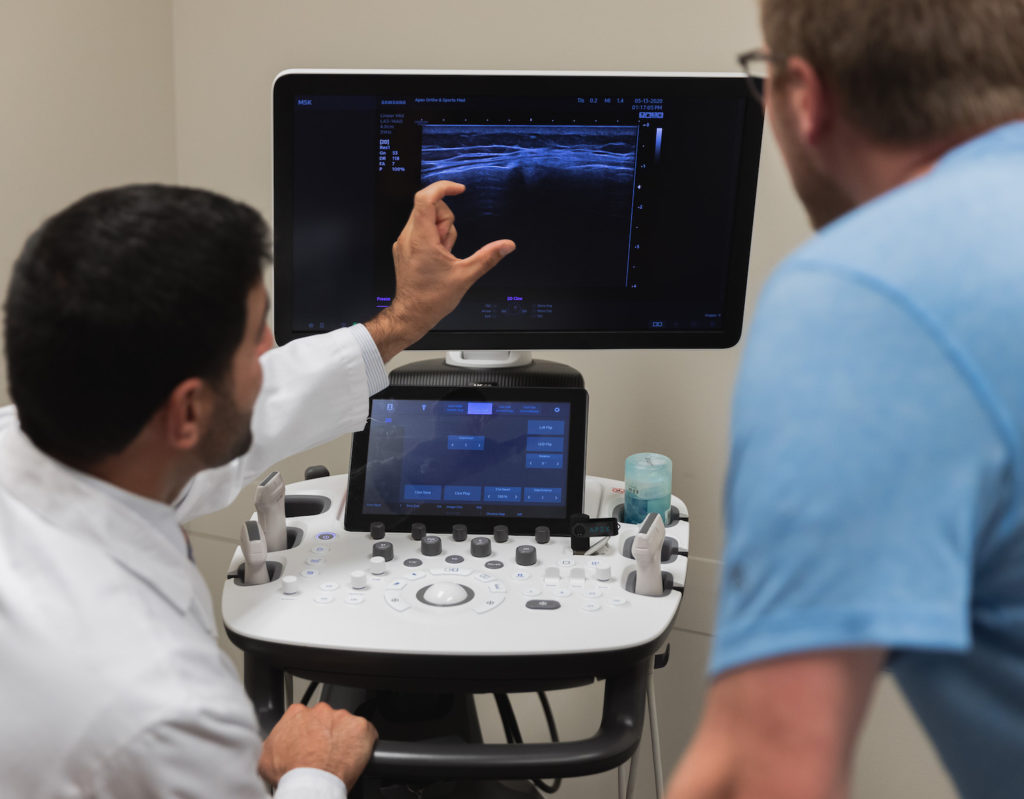
Ultrasound
From the diagnostic side, ultrasound is outstanding for diagnosing soft tissue and some bony conditions and often has a higher resolution than an MRI. Due to its higher resolution and dynamic scan capabilities (i.e. moving the shoulder during imaging), ultrasound offers an advantage over MRIs and CT scans.
A few common diagnoses via musculoskeletal ultrasounds include:
- Rotator cuff tears
- Hip bursitis
- Patellar tendonitis
- Ganglion cysts
- Ligament tears in the foot and ankle
- Tears in the knee
- Tennis elbow
- Impingement
- And more
Ultrasound also greatly improves the accuracy of injections. For example, glenohumeral injections in the shoulder miss their mark about 50% of the time without ultrasound imaging. But musculoskeletal ultrasound technology makes almost all injections approximately 99% accurate.
Regenerative medicine
Regenerative medicine involves treatments that use live cells, platelets, and other biologically active molecules to heal an injury.
Physicians like Dr. Khadavi and Dr. Moore who stay on top of the research curve understand that regenerative medicine and orthobiologics can treat many musculoskeletal conditions without surgery. For example, a cutting-edge stem cell treatment can help repair a rotator cuff injury that would have normally required a surgical fix.
As a result, orthobiologics allows doctors to treat patients with less pain, less rehabilitation, and less expense. Plus, regenerative treatments are nearly risk-free. The risk for a major complication is about 7 in 1,000,000, while the same risk from surgery is between 1 to 2%.
Regenerative treatments can heal and/or improve:
- Rotator cuff tears
- Hip bursitis
- Patellar tendonitis
- Ganglion cysts
- Ligament tears in the foot and ankle
- Tears in the knee
- Tennis elbow
- Impingement
And more
Electrodiagnostic studies
Electrodiagnostic studies help to measure the function of the nerves and comprise two portions:
- Nerve conduction study (NCS): sending small shocks down a nerve to assess its ability to carry information
- Electromyogram (EMG): placing small needles in the muscles to evaluate messages from the nerves for abnormalities
The information received from electrodiagnostic studies is like piecing a puzzle together to solve a problem. Therefore, the length of the study depends on two factors:
The complexity of the question: For example, is your study simply meant to rule out carpal tunnel syndrome, or is it also to evaluate for underlying radiculopathy? The latter will take longer to perform than the first.
How obvious or complex the findings are: In some cases, your physician may require more information from other nerves to reveal a specific pattern that suggests a definitive diagnosis.
Arthroscopy
Arthroscopy is a scope-based surgery used for the hip, knee, shoulder, and even elbow. Unlike open surgery, arthroscopy procedures don’t require large incisions, which can make healing, recovery, and pain management easier. With an arthroscopy, your provider can treat and repair a variety of sports-related conditions.
We understand that surgery may be a scary choice, but a vast majority of patients who undergo an arthroscopy can recover at 100%. To maximize your chances for an optimal outcome, it’s best to get as healthy as possible before you proceed with any type of surgery.
We require physical therapy after surgery, as it’s crucial for building strength and getting motion back.
For the top sports medicine clinic in Kansas City, visit Kansas City Orthopedic Alliance
The core of our success lies in proper diagnosis. An appointment with one of our providers includes the highest quality technology to pinpoint a patient’s underlying musculoskeletal conditions. From there, we can better understand which treatment will work best for you.
KCOA’s private practice model ensures our physicians can provide patients with the most value that doesn’t involve hidden fees or outlandish pricing.
For a thorough evaluation, call us at 913.319.7600 or schedule an appointment today.